Putting a Spotlight On

Each month The Arc of New Jersey Family Institute spotlights a different developmental disability to help build awareness and educate others about the disability. Learn more below.
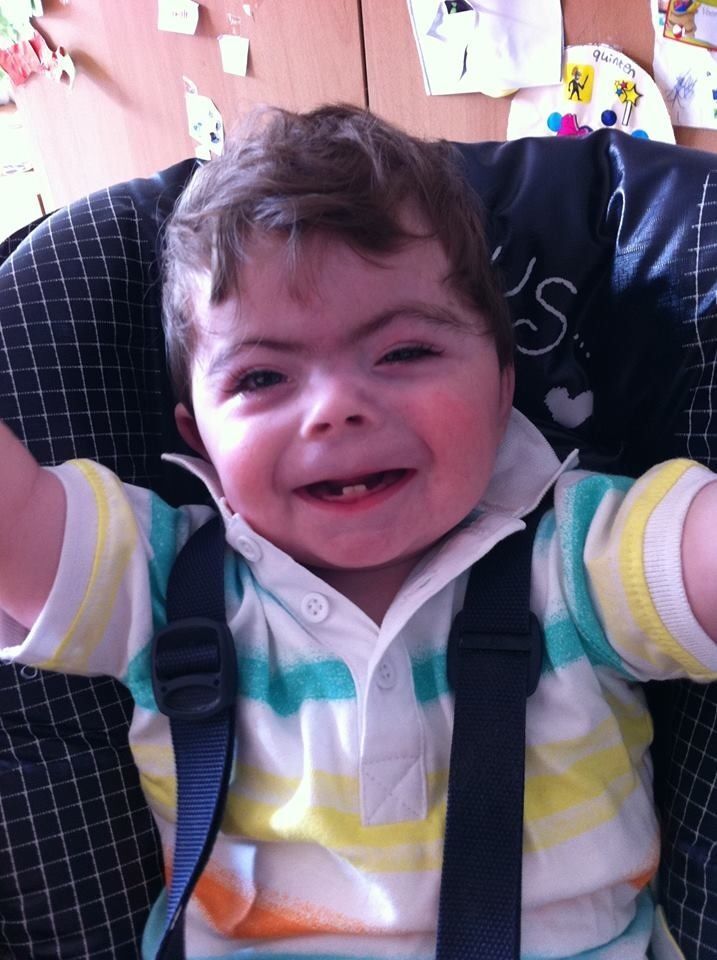
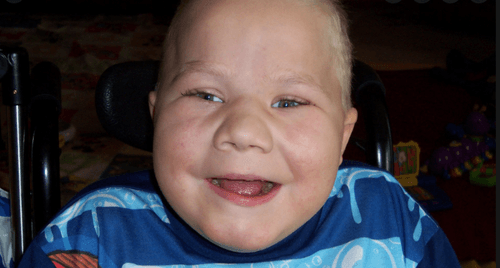
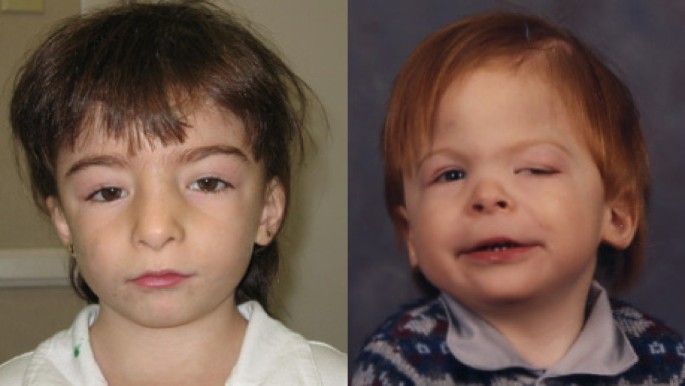
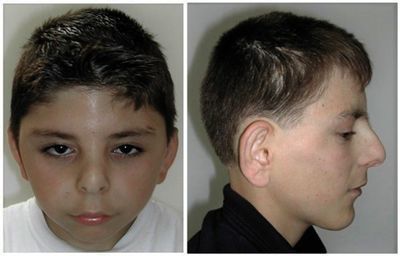
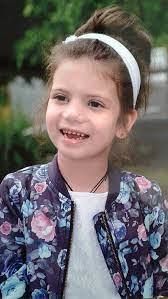
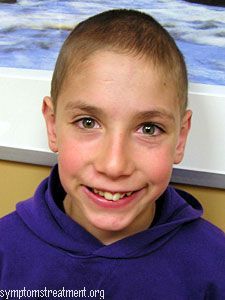
What is Cornelia de Lange Syndrome?
- Cornelia de Lange Syndrome is a rare genetic condition that affects growth and development and can range from mild to severe.
What are the signs/symptoms?
- malformations of the hands and arms
- microcephaly
- seizures
- autism spectrum disorders
- underdevelopment of the sexual organs
- cleft palate
- high, arched eyebrows, or eyebrows that meet in the midline
- widely spaced teeth or eyes
- hearing loss
- myopia
- & more
What is Cornelia de Lange Syndrome a result of?
- Cornelia de Lange Syndrome is caused by mutations in at least five genes (NIPBL, RAD21, SMC3, HDAC8, and SMC1A). The severity of the condition can vary greatly depending on the type of mutation and which gene is affected. More than half of people with CdLS have mutations in the NIPBL gene. This is also associated with more severe disease.
What are the complications of Cornelia de Lange Syndrome?
- Motor Dysfunction
- Social/ Bheavioral Comcerns
- Heart Problems
- Hearing Problems
- And more ...
References:
- https://www.ncbi.nlm.nih.gov/books/NBK1104/
- https://www.childrenshospital.org/conditions/cornelia-de-lange-syndrome